Clinical Corner
by Vikram Shankar, MD
Recently, I missed out. Tribal Health’s Nurse Supervisor Jamie Keppel and Security Officer Ken Franks led a simulation training. They simulated the case of a patient with organophosphate poisoning presenting to our Emergency Department. I wasn’t in the ED at the time, and I feel guilty for not being able to attend. These activities were routine in my residency—we ran through simulated cases, codes, and procedures on a near-daily basis. That experience was profoundly valuable—and missing out on last week’s sim spurred me to write about why I believe simulation training and experiential learning are so valuable.
I’d like to reflect on why simulation-based learning works and how we can embrace it even more. A large body of literature has shown that simulation supports quality improvement in (at least) these areas:
- Enhancing non-technical team-building skills [i]
- Helping staff master rare procedures [ii]
- Identifying latent safety threats and reducing patient safety events [iii] [iv]
- Identifying systems issues [v]
- Testing staff adherence to guidelines [vi] [vii]
Experiential learning fosters a supportive educational environment. I’ve seen these benefits both inside and outside the hospital setting.

Collaboration and Contribution
Simulation allows us to learn from each other. We each come to the exercise with different skills and experience. Maybe you bring the strong clinical gestalt of a seasoned physician. Or perhaps you have the ultrasound knowledge of someone just out of residency. We all have something to contribute, and simulation-based learning provides a setting for us to play our parts.
In daily practice, we sometimes follow established algorithms. When a stroke alert comes in, we do exactly what we were trained to do: Assess the airway, go to the CT scanner, consider thrombolytics, and get the patient dispositioned appropriately. The natural tendency for many of us is to make decisions—unintentionally perhaps—in our own personal silos.
But what if we recreated the stroke alert in a simulation? We could deconstruct the process in a collaborative way. How might we behave differently, knowing we had room to experiment and examine each step?
Perhaps we could:
- Workshop and fine-tune our understanding of the NIHSS scale together. How is limb ataxia scored in a person with a weak limb? Does an initial subtle correction in motor drift technically count as a drift?
- Review TPA criteria as a team.
- Identify hidden roles. Who is putting in orders? Who is calling radiology? Who is mobilizing air transportation?
- Evaluate our performance of time-critical metrics. What is the door-to-CT time, door-to-TPA time, and so on?
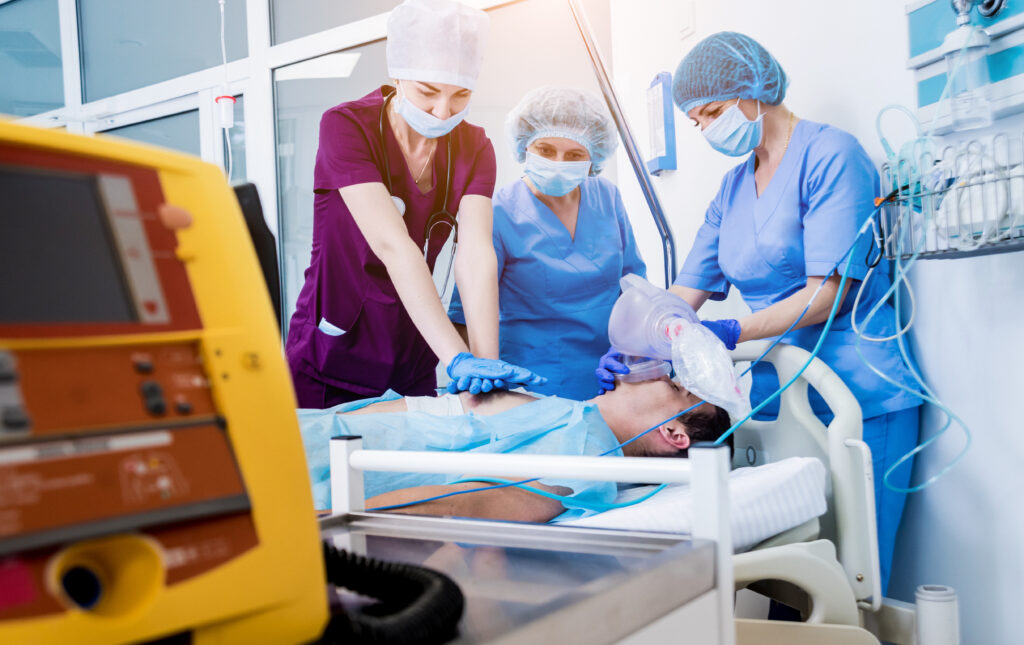
The Benefits of Post-Simulation Debriefing
Beyond that clear opportunity, there’s a second component that I think is sometimes even more valuable. This is the post-simulation debriefing session. That session is an opportunity to discharge the team’s emotional buildup from the activity, process the case, and review relevant clinical content. And it really does help! Some simulation experts argue that debriefing is even more valuable than the simulation itself. Feeling acknowledged and appreciated by other members of a team goes a long way toward strengthening relationships, breaking down communication barriers, and reinforcing good medical decision-making. Yes, the simulation itself has intrinsic value—but thoughtful discussion of that simulation is key to completing the process.
Going beyond the boundaries of the hospital, experiential learning allows us to connect better with our local community. I recently sat down with leaders from our hospital who are well-acquainted with challenges facing our community. One challenge they mentioned is that there are few avenues for community members to pursue higher levels of training. I don’t pretend to have particular insight into the upstream determinants of health—such as poverty—that afflict our community. But I do know that we as healthcare providers have specialized knowledge and training that can be a source of connection.
Looking back on my own residency, I see a path to help the community we serve. In my residency, we invited students from local high schools who had an interest in healthcare and medicine to our simulation/procedure lab. That served two functions: First, students got a visceral sense of the work—and this could actually steer their careers.
Second, the activity offered students respite from potentially challenging home environments. In a resource-poor setting, where it’s hard to conceive of the amount of blocked opportunity the average person faces, I think we’re uniquely situated to help our community. Experiential learning could take the form of a procedure lab—we could go over basic suturing skills or basic CPR training with students who might pursue careers in healthcare. Or students could participate in a simulated cardiac arrest, learning how to hook a patient up to a monitor and perform chest compressions. Even if the outcome for a given student is not a career in healthcare, this experience builds bridges with the community.
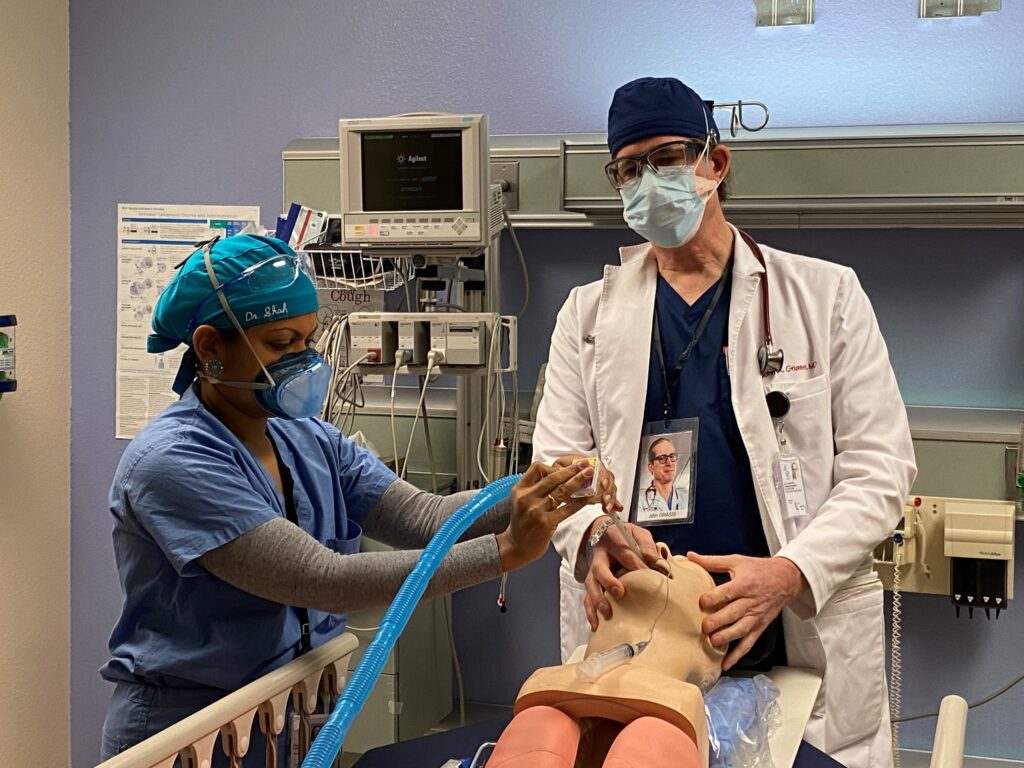
Fostering Personal, Professional, and Team Growth
I also need to acknowledge the obvious: Simulation and experiential learning aren’t universally beloved. Some people enjoy simulation and others find it uncomfortable. When you’re the one on the spot—leading a simulated cardiac arrest, for example—it exposes your knowledge gaps in a way that can be embarrassing. How do we solve this? Ultimately, it’s an issue of culture—the set of expectations around the activity, and the permission we give one another to be vulnerable.
To make simulation more attractive, we have to acknowledge its inherent awkwardness. Then we work to make it a more inviting atmosphere. I suggest applying Las Vegas rules: What happens in the sim lab stays in the sim lab. It must be a profoundly safe environment, where people are encouraged to ask questions, take risks, and even make mistakes. The sim lab is a tool that fosters personal, professional, and team growth without risking lives. I believe we should embrace it further.
I’m kicking myself for not attending Jamie’s sim session last week. But I hope there will be more to come, especially in our new ED. Simulation and experiential learning are processes we are all equipped to engage in. They are paths to build connections among providers, across specialties, and even between ourselves and the community we serve. I’ll be there next time.
[i] Wheeler DS, Geis G, Mack EH, LeMaster T, Patterson MD. High-reliability emergency response teams in the hospital: improving quality and safety using in situ simulation training. BMJ Qual Saf. 2013 Feb 1:bmjqs-2012.
[ii] Petrosoniak A, Ryzynski A, Lebovic G, Woolfrey K. Cricothyroidotomy In Situ Simulation Curriculum (CRIC Study): Training Residents for Rare Procedures. Simulation in Healthcare. 2017 Apr 1;12(2):76-82.
[iii] Patterson MD, Geis GL, LeMaster T, Wears RL. Impact of multidisciplinary simulation-based training on patient safety in a paediatric emergency department. BMJ Qual Saf. 2012 Dec 1:bmjqs-2012.
[iv] Petrosoniak A, Auerbach M, Wong AH, Hicks CM. In situ simulation in emergency medicine: moving beyond the simulation lab. Emergency Medicine Australasia. 2017 Feb 1;29(1):83-8.
[v] Moreira ME, Hernandez C, Stevens AD, Jones S, Sande M, Blumen JR, Hopkins E, Bakes K, Haukoos JS. Color-coded prefilled medication syringes decrease time to delivery and dosing error in simulated emergency department pediatric resuscitations. Annals of emergency medicine. 2015 Aug 31;66(2):97-106.
[vi] Qian J, Wang Y, Zhang Y, Zhu X, Rong Q, Wei H. A Survey of the first-hour basic care tasks of severe sepsis and septic shock in pediatric patients and an evaluation of medical simulation on improving the compliance of the tasks. The Journal of emergency medicine. 2016 Feb 29;50(2):239-45.
[vii] Kessler DO, Walsh B, Whitfill T, Gangadharan S, Gawel M, Brown L, Auerbach M. Disparities in adherence to pediatric sepsis guidelines across a spectrum of emergency departments: a multicenter, cross-sectional observational in situ simulation study. The Journal of emergency medicine. 2016 Mar 31;50(3):403-15

